Physical Examination
The doctor will perform a physical exam to determine diagnosis. He will be looking for common features reported in RA, including:
- Joint swelling
- Joint tenderness
- Loss of motion in your joints
- Joint mal-alignment
- Signs of rheumatoid arthritis in other organs, including your skin, lungs and eyes.
- Complete Blood Count
- Erythrocyte Sedimentation Rate (ESR)
- C-Reactive Protein
- R A factor
- Anti CCP-ANA
Antinuclear Antibodies (ANA)
This test detects a group of autoantibodies (antibodies against self), which is seen in about 30 to 40 percent of people with RA. Although it commonly is used as a screening tool, ANA testing isn’t used as a diagnostic tool because many people without RA or with other diseases can have ANAs.
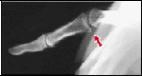
Imaging Studies
- Radiographs (X-rays)
- Magnetic Resonance Imaging (MRI)
- Joint Ultrasound
Treatment options
Because rheumatoid arthritis presents itself on many different fronts and in many different ways, treatment must be tailored to the individual, taking into account the severity of your arthritis, other medical conditions you may have and your individual lifestyle. Current treatment methods focus on relieving pain, reducing inflammation, stopping or slowing joint damage and improving your functioning and sense of well-being.
Rheumatoid arthritis is a serious disease. It is crucial that you get an early diagnosis and work with your doctor to find the best treatment for you so that you can live well with it.
Medications
The proper medication regimen is important in controlling your RA. You must help your doctor determine the best combination for you. The main categories of drugs used to treat RA are:
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) – These drugs are used to reduce inflammation and relieve pain. These are medications such as aspirin, ibuprofen, indomethacin and aceclofenac/diclofenac.
Analgesic Drugs – These drugs relieve pain, but don’t necessarily have an effect on inflammation. Examples of these medications are acetaminophen, propoxyphene, mepeidine and morphine.
Glucocorticoids or Prednisone – These are prescribed in low maintenance doses to slow joint damage caused by inflammation.
Disease Modifying Antirheumatic Drugs (DMARDs) – These are used with NSAIDs and/or prednisone to slow joint destruction caused by RA over time. Examples of these drugs are methotrexate, injectable gold, penicillamine, azathioprine, chloroquine, hydroxychloroquine, sulfasalazine and oral gold.
Biologic Response Modifiers – These drugs directly modify the immune system by inhibiting proteins called cytokines, which contribute to inflammation. Examples of these are etanercept, infliximab, adaliumumab and anakinra.
Protein-A Immuoadsorption Therapy – This is not a drug, but a therapy that filters your blood to remove antibodies and immune complexes that promote inflammation.
DMARDs, particularly methotrexate, have been the standard for aggressively treating RA. Recently, studies have shown that the most aggressive treatment for controlling RA may be the combination of methotrexate and another drug, particularly biologic response modifiers. The dual drug treatment seems to create a more effective treatment, especially for people who may not have success with or who have built up a resistance to, methotrexate or another drug alone. Doctors now are prescribing combination drug therapy more often and studies continue. It appears that these combination drug therapies might become the new road to follow in treating RA. Here are some medications your doctor may suggest you combine with methotrexate: lefluonomide (Arava), etanercept (Enbrel), adalimumab (Humira) and infliximab (Remicade).
Surgery