-
Mon - Sat
08:00am - 08:00pm

Osteoarthritis is the most common form of arthritis.
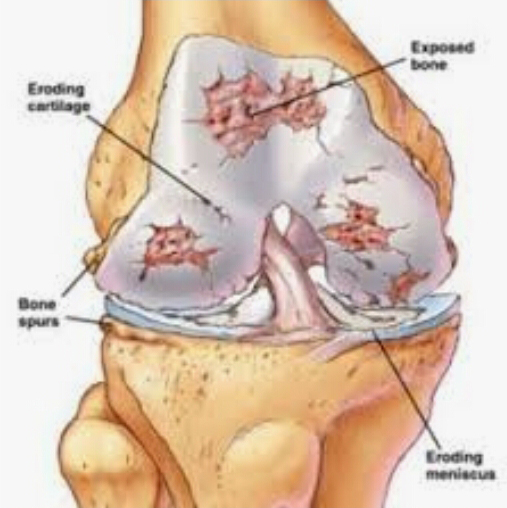
It is caused by the breakdown of cartilage. Cartilage is the tough elastic material that covers and protects the ends of bones. Bits of cartilage may break off and cause pain and swelling in the joint between bones. This pain and swelling is called inflammation.
Over time the cartilage may wear away entirely, and the bones will rub together.
Osteoarthritis can affect any joint but usually affects hips, knees, hands and spine.
Cartilage is the tough elastic material that covers and protects the ends of bones. In healthy joints cartilage acts as a shock absorber when you put weight on the joint. The slippery surface of the cartilage allows the bones to move smoothly. When a joint develops osteoarthritis the cartilage gradually becomes rough and thin, and the bone underneath thickens.
Pain, stiffness and swelling around a joint that lasts longer than two weeks. The joints that are usually affected are the hips, knees, feet and spine and thumb joints might also be affected.
If you are experiencing persistent joint pain, visit the orthopaedic surgeon at AOSM center.
Damage due to OA progresses slowly over time and may result in several problems. You may have pain, especially when moving a joint. Sometimes, you may hear a grinding sound when the roughened cartilage on the surface of the bones rubs together. A joint may feel sore and stiff, and the joint won’t move as easily or as far as it once did. All these changes can make it hard to move around and to do everyday tasks, pain after long sitting, standing or walking up stairs.
If you are experiencing persistent joint pain, visit your family doctor at A+OSM Center. Describe the pain in detail including where the pain occurs and when.
The x-ray is the most useful test to confirm osteoarthritis.
OA. Key risk factors include: heredity; excess weight; injury; joint damage from another type of arthritis.
If the doctor at A+OSM Center thinks you have osteoarthritis, he or she may perform a physical examination and order tests such as x-rays.
Although there is no cure for osteoarthritis, there are a number of steps you can take to manage your pain and lead an active life.
Establishing the correct diagnosis is very important, because something can be done to manage most forms of arthritis, and most therapies work best when started early in the disease.
Your doctor may be able to diagnose OA based on your medical history and a physical examination. Sometimes, your doctor may order certain tests to help confirm the diagnosis, to determine how much joint damage exists, or to distinguish among different types of arthritis. These tests may include x-rays, blood tests or joint fluid tests.
Although there is no cure for OA, a lot can be done to help manage the condition. A variety of treatments can help to lessen pain and stiffness and to make movement easier. Your active involvement in developing your prescribed treatment plan is essential.
Acetaminophen is often the first medication chosen to treat osteoarthritis. It can relieve pain but does not reduce inflammation.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
First line management
Nonsteroidal anti-inflammatory drugs (NSAIDs) are a type of medication that helps reduce the pain and swelling of the joints and decrease stiffness. However, they do not prevent further joint damage.
Exercise helps reduce pain and prevents further joint damage. It can also help you maintain a healthy weight, which puts less strain on your joints.
Not using a sore joint will cause the muscles around it to become weak, resulting in pain.
A physiotherapist can teach you correct exercises such as:
Strengthening exercises improve muscle strength and tone, which will help to stabilize and protect osteoarthritic joints and reduce the pain.
Range of motion exercises help maintain or restore normal joint movement and relieve stiffness.
Low impact exercises such as walking and swimming, which do not put unnecessary strain on joints.
Muscles and the other tissues that hold joints together weaken when they aren’t moved enough, so the joint loses its shape and function. Exercise helps lessen the symptoms of OA and can help make you feel better overall. Moderate stretching exercises will help relieve the pain and keep the muscles and tendons around the affected joint more flexible and strong. Low-impact exercises like swimming, walking, water aerobics and stationary bicycling can all reduce pain while maintaining strength and flexibility.
Positioning joints wisely helps you use them in ways that avoid extra stress. Use larger, stronger joints to carry loads. For example, use a shoulder bag instead of a hand-held one. Also, avoid keeping the same position for a long period of time.
Applying heat helps relax aching muscles, and reduces joint pain and soreness.
Applying cold helps to lessen the pain and swelling in a joint.
Heat applied to an arthritic area can reduce pain, stiffness and muscle spasm. It promotes blood circulation, which nourishes and detoxifies muscle fibers. Having a hot shower before exercise may help you get ready for the workout. You should not apply heat to an inflamed joint. Cold applied to inflamed joints reduces pain and swelling by constricting blood flow.
Another treatment is viscosupplementation, in which a clear gel-like substance is injected into the knee. This substance lubricates the cartilage (much like oil lubricates an engine), reducing pain and allowing greater movement of the knee.
Viscosupplementation restores frictionless movement within the joint, thus reducing pain and allowing greater mobility.
If one of your joints becomes badly damaged, or if the pain is too strong, your doctor may recommend surgery.
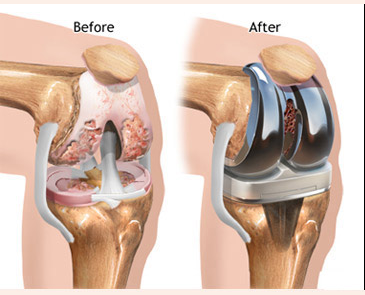
There are different kinds of surgery for OA. With some surgery, bits of cartilage are removed from the joint. Other kinds of surgery repair or rebuild parts of the bone, or replace a joint with an artificial or a man-made joint. (see total knee replacement surgery)
Osteoarthritis may progress to the point where surgery is necessary. Minor surgery can be performed to clean out cartilage debris from the joints, particularly the knee. This is called arthroscopic surgery. It is performed as outpatient surgery and does not usually require an overnight stay in hospital. Severely damaged joints can be reconstructed or surgically replaced with artificial ones called as Joint replacement surgery, and is most often performed to replace hip and knee joints. Artificial joints can last 10-20 years before they require replacement, this is why this type of surgery is delayed until it is clearly necessary.
Reduce pain and inflammation, improve joint function and slow disease progression. Slow deterioration of cartilage, relieve osteoarthritis pain and improve joint mobility. Reduce pain and inflammation.